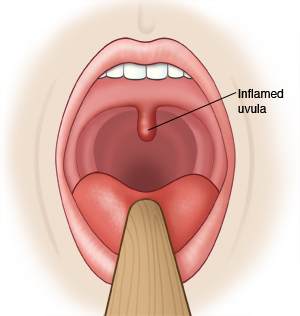
The uvula is the tissue that hangs in the back of the throat. Uvulitis is inflammation of the uvula. Inflammation happens when the body responds to an injury, allergic reaction, infection, or illness. Symptoms of inflammation may include redness, irritation, itching, swelling, or burning. Uvulitis is more common in children than adults.
Symptoms of uvulitis may include:
-
Sore throat.
-
Trouble swallowing.
-
Painful swallowing.
-
Trouble breathing.
Possible causes of uvulitis include:
-
Throat infection.
-
Inhaling or swallowing chemicals.
-
Inhaling hot air or steam.
-
Allergic reaction to something eaten, touched, or breathed in.
-
Post general anesthesia where a breathing tube was put in.
In rare cases, uvulitis can be caused by a condition called angioedema. Angioedema can be:
-
Hereditary (runs in the family).
-
An allergic reaction.
-
A reaction to some medicines, including aspirin and nonsteroidal anti-inflammatories (NSAIDs), such as ibuprofen.
-
A side effect of a class of drugs used for high blood pressure called ACE inhibitors.
-
Life-threatening. It can lead to swelling of the air passage in the mouth or throat. Severe swelling can block your breathing and cause death. Watch for the earliest signs of this illness. Call
911 if the swelling involves the face, mouth, or throat areas.
To help find the cause of the uvulitis, imaging tests may be done. If infection is suspected, swabs from the throat or samples of blood may be tested. Questions may be asked about a person’s immunization history to be sure it is up to date. A cause for uvulitis is not always found.
Treatment depends on the cause and the severity of the symptoms.
Home care
Medicines
The health care provider may prescribe antibiotics for a bacterial infection. For an allergic reaction or angioedema, medicines called steroids, epinephrine, or antihistamines may be given. Follow instructions when using any medicine.
General care
To care for uvulitis at home:
-
Rest until the symptoms go away.
-
If medicines were prescribed, be sure they are taken as directed. They should be taken until they are gone or when the health care provider says to stop them.
-
If you were told that your angioedema was from a medicine that you are taking, you must stop taking this medicine. Contact your provider for a prescription for a different medicine. Advise future providers that you are allergic to this medicine. Consider wearing a medical alert bracelet or necklace. Make sure the medicine allergy is clearly identified in your health records.
-
Contact your provider before taking any over-the-counter medicines.
-
Drink fluids. Pain when swallowing may make it harder to drink and lead to dehydration. To prevent this, sip fluids throughout the day. Children can be given frozen juice bars, milk, or other cold liquids. Watch for the signs of dehydration listed below.
-
Avoid alcohol and sedatives.
-
Use a humidifier, especially when indoor heating is on
-
Ask your provider when you can return to work or school. Ask your child’s provider when your child can return to school or child care.
Follow-up care
Follow up with the health care provider, or as directed. You may be referred to an allergy doctor or an ear, nose, and throat doctor (ENT or otolaryngologist) for further evaluation and treatment. Make these visits as soon as possible.
When to get medical advice
Contact the health care provider right away if:
-
Symptoms are not going away or are getting worse.
-
Symptoms of dehydration occur, including dark urine, dry mouth, cracked lips, dizziness, or sunken eyes.
-
Your child is acting very sick or not improving.
-
You are an adult and have a fever over 100.4°F (38°C), or as directed by your provider.
-
Your child has a fever (see "Fever and children" below).
Call 911
Call
-
Drooling or trouble swallowing
-
Trouble breathing
-
Trouble talking
-
Swollen tongue, lips, face, or throat. You can tell this is happening if your child's voice changes.
-
Jerking and loss of consciousness; seizure
-
Lack of response, extreme drowsiness, or trouble waking up
-
Fainting
-
Confusion
-
Child being unresponsive
-
Skin or lips look blue, purple, or gray
Fever and children
Use a digital thermometer to check your child’s temperature. Don’t use a mercury thermometer. There are different kinds and uses of digital thermometers. They include:
-
Rectal. For children younger than 3 years, a rectal temperature is the most accurate.
-
Forehead (temporal). This works for children age 3 months and older. If a child under 3 months old has signs of illness, this can be used for a first pass. The health care provider may want to confirm with a rectal temperature.
-
Ear (tympanic). Ear temperatures are accurate after 6 months of age, but not before.
-
Armpit (axillary). This is the least reliable but may be used for a first pass to check a child of any age with signs of illness. The provider may want to confirm with a rectal temperature.
-
Mouth (oral). Don’t use a thermometer in your child’s mouth until he or she is at least 4 years old.
Use the rectal thermometer with care. Follow the product maker’s directions for correct use. Insert it gently. Label it and make sure it’s not used in the mouth. It may pass on germs from the stool. If you don’t feel OK using a rectal thermometer, ask the provider what type to use instead. When you talk with any provider about your child’s fever, tell him or her which type you used.
Below are guidelines to know if your young child has a fever. Your child’s provider may give you different numbers for your child. Follow your provider’s specific instructions.
Fever readings for a baby under 3 months old:
-
First, ask your child’s provider how you should take the temperature.
-
Rectal or forehead: 100.4°F (38°C) or higher
-
Armpit: 99°F (37.2°C) or higher
Fever readings for a child age 3 months to 36 months (3 years):
-
Rectal, forehead, or ear: 102°F (38.9°C) or higher
-
Armpit: 101°F (38.3°C) or higher
Contact the health care provider in these cases:
-
Repeated temperature of 104°F (40°C) or higher in a child of any age
-
Fever of 100.4° F (38° C) or higher in baby younger than 3 months
-
Fever that lasts more than 24 hours in a child under age 2
-
Fever that lasts for 3 days in a child age 2 or older