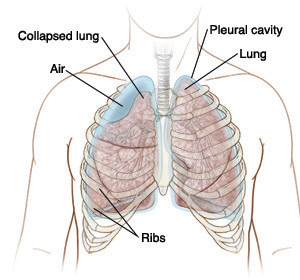
Pneumothorax happens when air leaks out of a lung and gets trapped in the space between the lung and the chest wall (pleural space). It can cause complete or partial collapse of a lung. The trapped air prevents the lung from re-inflating. Spontaneous pneumothorax happens when a weakened spot on the lung surface (“bleb”) ruptures. It may occur in people with asthma or emphysema, or even in those with no pre-existing lung disease.
If your pneumothorax is small, it should get better without treatment and can be managed at home. If the amount of trapped air grows larger, it must be removed with a tube (catheter) placed into the pleural space.
Home care
-
Rest at home. Don't do vigorous activity or exercise. Speak with your health care provider about when it's safe to start exerting yourself again.
-
Use over-the-counter pain medicine to control pain unless another medicine was prescribed. Use only the prescribed amount. (Talk with your provider before using them if you have chronic liver or kidney disease or have ever had a stomach ulcer or gut bleeding. Also, talk to your provider if you are taking medicine to prevent blood clots.)
-
During the next
3 days, take4 slow, deep breaths every1 to 2 hours while awake. Do this even though your chest may hurt when you breathe. It sends extra oxygen and blood to the lung. This is important to help keep the lung expanded. If the provider gave you a breathing exercise device (incentive spirometer), use it as directed. -
If you smoke or use e-cigarettes, quit. Ask your provider for help.
-
Stay away from secondhand smoke. Don't let anyone smoke in your house or car.
Follow-up care
Follow up with your provider, or as advised, for a repeat chest X-ray to be sure the pneumothorax is not getting larger.
If X-rays were taken, you will be told of any new findings that may affect your care.
Call 911
Call
-
Your breathing gets more difficult.
-
You have confusion, dizziness, or difficulty waking up.
-
You faint or lose consciousness.
-
You have a rapid heart rate.
-
You feel new pain in your chest, arm, shoulder, neck, or upper back.
-
Your lips or skin look blue, purple, or gray in color.
-
You have a feeling of doom.
When to contact your doctor
Contact your provider right away if:
-
You have more pain with breathing.
-
You feel weak.
-
You have a fever of 100.4ºF (38ºC) or higher, or as directed by your provider.
-
You cough up sputum.