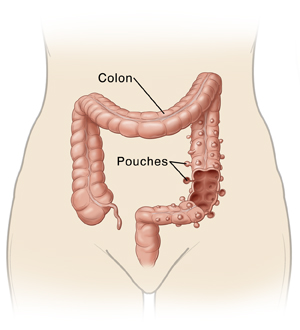
Diverticulosis means that small pouches have formed in the wall of your large intestine (colon). The pouch-like structures, or diverticula, arise from the areas of muscle weakness in the colon. Most often, this problem causes no symptoms and is common as people age. But the pouches in the colon are at risk of becoming infected. When this happens, the condition is called diverticulitis. Although most people with diverticulosis never develop diverticulitis, it's still not uncommon. Rectal bleeding can also occur and in less common situations, a type of colon inflammation called colitis.
Most people don't have symptoms. But some people with diverticulosis may have:
-
Belly (abdominal) cramps and pain
-
Bloating
-
Change in bowel habits (diarrhea or constipation)
Causes
The exact cause of diverticulosis (and diverticulitis) has not been proven, but a few things are linked with the condition:
-
Low-fiber diet. But some experts don't agree about this.
-
Constipation
-
Lack of exercise
Your healthcare provider will talk with you about how to manage your condition. Diet changes may be all that you need to help control diverticulosis and prevent it from becoming diverticulitis. If you develop diverticulitis, you will likely need other treatments.
Home care
You may be told to take fiber supplements daily. Fiber adds bulk to the stool so that it passes through the colon more easily. Stool softeners may also be recommended. You may also be given medicines for pain relief. Be sure to take all medicines as directed.
In the past, people were told to not have corn, nuts, or seeds. You no longer need to do this.
Follow these guidelines when caring for yourself at home:
-
Eat unprocessed foods that are high in fiber. Whole grains, fruits, and vegetables are good choices.
-
Drink 6 to 8 glasses of water every day unless your healthcare provider has you limit how much fluid you should have.
-
Watch for changes in your bowel movements. Tell your provider if you notice any changes.
-
Begin an exercise program. Ask your provider how to get started. Generally, walking is the best.
-
Get plenty of rest and sleep.
Follow-up care
Follow up with your healthcare provider, or as advised. You may need regular visits to check on your health. Sometimes you may need special procedures, such as colonoscopy or sigmoidoscopy. Be sure to keep all your appointments.
If a stool sample was taken, or cultures were done, you'll be told if they are positive, or if your treatment needs to be changed. You can call as directed for the results.
If X-rays were done, you'll be told of any new findings that may affect your care.
If antibiotics were prescribed, be sure to finish them all.
When to get medical advice
Call your healthcare provider right away if any of these occur:
-
Fever of 100.4°F (38°C) or higher , or as directed by your healthcare provider
-
Severe cramps in the belly (abdomen) or pain that's getting worse
-
Tenderness in the lower left side of the abdomen or pain throughout the abdomen that gets worse
-
Diarrhea or constipation that doesn't get better within 24 hours
-
Nausea and vomiting
-
Slight bleeding from the rectum or black, tarry stools
Call 911
Call
-
Large amount of bleeding from the rectum
-
Trouble breathing
-
Confusion
-
Very drowsy or trouble awakening
-
Fainting or loss of consciousness
-
Rapid heart rate
-
Chest pain
-
Sudden, severe belly pain
Featured in