Everyone has had a cough as part of the common cold, flu, or bronchitis. This kind of cough occurs along with an achy feeling, low-grade fever, nasal and sinus congestion, and a scratchy or sore throat. This usually gets better in 2 to 3 weeks. A cough that lasts longer than 8 weeks may be due to other causes. Your health care provider may refer to this as a chronic cough.
If your cough does not improve over the next 2 weeks, further testing may be needed. Follow up with your health care provider as advised. Cough suppressants may be recommended. Based on your exam today, the exact cause of your cough is not certain. Below are some common causes of a chronic cough.
Smoker's cough
A smoker’s cough doesn’t go away. If you continue to smoke, it only gets worse. The cough is from irritation in the air passages. Talk to your health care provider about quitting. Medicines or nicotine-replacement products, like gum or the patch, may make quitting easier.
Postnasal drip
A cough that is worse at night may be due to postnasal drip. Excess mucus in the nose drains from the back of your nose to your throat. This sets off the cough reflex. Postnasal drip may be due to a sinus infection or allergy. Common allergens include dust, tobacco smoke (both inhaled and secondhand smoke), environmental pollutants, pollen, mold, pets, cleaning agents, room deodorizers, and chemical fumes. Over-the-counter antihistamines or decongestants may be helpful for allergies. A sinus infection may need antibiotic treatment. See your health care provider if symptoms continue.
Medicines
Certain prescribed medicines can cause a chronic cough in some people:
-
ACE inhibitors for high blood pressure. These include enalapril, lisinopril, and others.
-
Beta-blockers for high blood pressure and other conditions. These include propranolol, metoprolol, and others.
Let your health care provider know if you are taking any of these. A chronic cough may mean your medicine needs to be changed.
Asthma
A cough may be the only sign of mild asthma. You may have tests to find out if asthma is causing your cough. You may also take asthma medicine on a trial basis.
Acid reflux (heartburn, GERD)
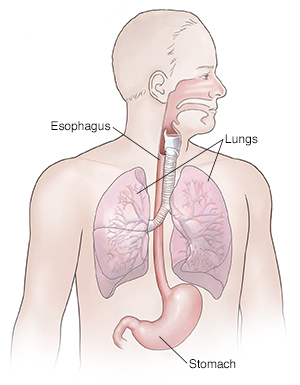
The esophagus is the tube that carries food from the mouth to the stomach. A valve at its lower end prevents stomach acids from flowing upward. If this valve does not work correctly, acid from the stomach enters the esophagus. This may cause a burning pain in the upper abdomen or lower chest, belching, or cough. Symptoms are often worse when lying flat. Stay away from eating or drinking before bedtime. Try using extra pillows to raise your upper body, or place 4-inch blocks under the head of your bed. You may try an over-the-counter (OTC) antacid or an acid-blocking medicine, such as cimetidine, or omeprazole. Stronger medicines for this condition can be prescribed by your health care provider. Ask your provider which OTC medicine to use. Depending on your current medicines, some OTC medicines may cause drug interactions and should not be used.
Follow-up care
Follow up with your health care provider, or as advised, if your cough doesn't improve. Further testing may be needed.
Note: If an X-ray is taken, you'll be informed of any new findings that may affect your care.
When to get medical advice
Contact your health care provider right away if any of these occur:
-
Mild wheezing or trouble breathing
-
Fever of 100.4ºF (38ºC) or higher, or as advised by your provider
-
Unexpected weight loss
-
Coughing up large amounts of colored sputum or blood-tinged sputum
-
Night sweats (sheets and pajamas get soaking wet)
Call 911
Call
-
Coughing up blood
-
Moderate to severe trouble breathing or wheezing